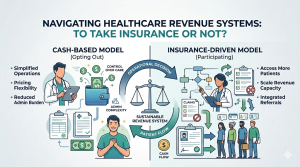
Traditional medical billing alone cannot maximize healthcare revenue because it begins after critical financial decisions have already been made. These traditional medical billing limitations mean that by the time a claim is submitted, factors like insurance eligibility, prior authorization, documentation, and coding have already determined reimbursement outcomes. This makes traditional billing a reactive, not preventative, function, where most revenue issues originate before claims are even created. As a result, organizations experience denials, delays, and revenue leakage despite efficient billing operations. To truly improve financial performance, healthcare practices must shift upstream, focusing on eligibility, authorization, coding accuracy, and documentation, while aligning the entire revenue cycle, because billing improvements alone lead to limited growth, whereas full system alignment drives higher collections and fewer denials.
In many healthcare organizations, medical billing is viewed as the primary driver of revenue performance. When financial results fall short of expectations, the most common response is to evaluate billing workflows, increase follow-up efforts, or invest in additional billing resources.
While these actions may improve certain aspects of collections, they often fail to address a more fundamental issue:
Medical billing, as it is traditionally defined, begins too late in the process to fully control revenue outcomes.
Traditional medical billing typically starts at the point of claim creation and submission, followed by payment posting, denial management, and collections. This model assumes that once a claim is generated, the primary challenge is ensuring it is processed and paid correctly.
However, by the time a claim reaches the billing stage, many of the factors that determine whether it will be paid and how much will be reimbursed have already been decided.
As a result, healthcare organizations that rely solely on traditional billing approaches often find themselves reacting to problems rather than preventing them.
Understanding the limits of traditional medical billing is essential for organizations seeking to improve financial performance, reduce denials, and capture the full value of the services they provide.
What Is Traditional Medical Billing?
Traditional medical billing focuses on the back-end financial processes that occur after a patient encounter has taken place. These processes typically include:
- Charge entry
- Claims submission
- Claim rejection management
- Denial management
- Accounts receivable follow-up
- Payment posting
- Patient billing and collections
Within this model, billing teams are responsible for ensuring that claims are submitted accurately and that payments are collected from both insurance payers and patients.
This function is critical. Without effective billing operations, healthcare organizations would struggle to convert services into revenue.
However, traditional billing operates within a limited scope.
It assumes that the information entering the billing process is correct, complete, and aligned with payer requirements.
In reality, this assumption is often incorrect.
The Core traditional medical billing Limitations: Billing Begins After Key Decisions Are Made
By the time a claim is created, several critical decisions have already been made that directly impact reimbursement:
- Whether the patient’s insurance was verified correctly
- Whether prior authorization was required and obtained
- Whether the provider was credentialed with the payer
- Whether the service is covered under the patient’s plan
- Whether clinical documentation supports medical necessity
- Whether coding accurately reflects the services delivered
If any of these elements are misaligned, the claim may be:
- Rejected before processing
- Denied by the payer
- Underpaid
- Delayed
At this point, billing teams can attempt to correct the issue, but they are no longer operating in a preventative capacity. They are operating in a reactive mode, attempting to recover revenue that has already been placed at risk.
Upstream Dependencies That Traditional Billing Does Not Control
Traditional medical billing does not typically include responsibility for several upstream functions that significantly influence revenue outcomes.
Insurance Eligibility and Benefit Verification
Before a patient is seen, it is essential to verify:
- Active insurance coverage
- Benefit details
- Deductible and copayment requirements
- Coverage limitations
If eligibility is not verified correctly:
- Claims may be rejected
- Patients may be billed incorrectly
- Reimbursement may be delayed
Billing teams often encounter these issues only after a claim has already failed.
Prior Authorization
Many services require prior authorization before they can be reimbursed. If authorization is not obtained:
- Claims may be denied regardless of medical necessity
- Appeals may be required
- Reimbursement may be delayed or lost entirely
Traditional billing does not control whether authorization was obtained correctly.
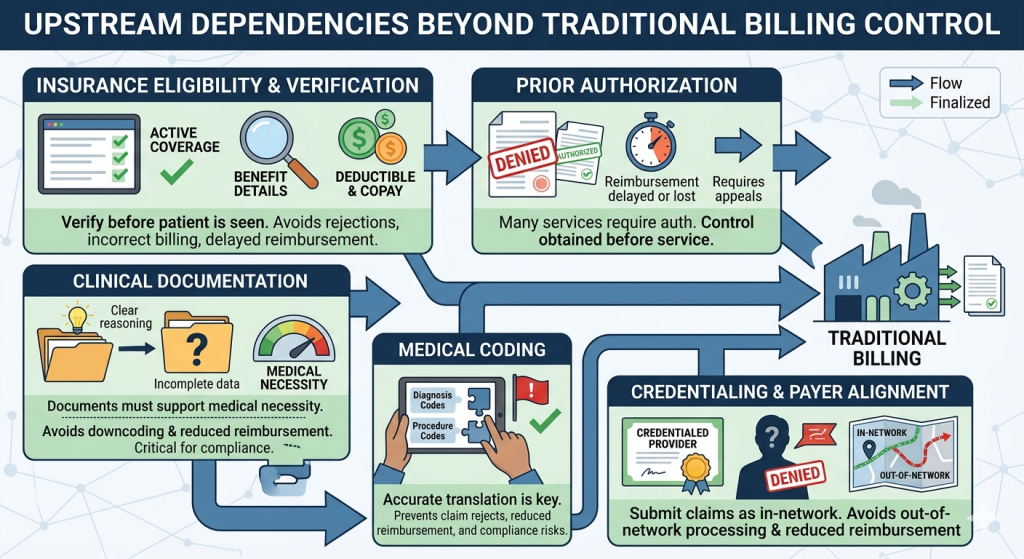
Clinical Documentation
Clinical documentation determines whether services meet payer requirements for medical necessity. If documentation is incomplete or inconsistent:
- Claims may be denied
- Services may be downcoded
- Reimbursement may be reduced
Billing teams rely on documentation that has already been completed and cannot fully correct deficiencies after the fact.
Medical Coding
Coding translates clinical services into billable claims. If coding is inaccurate:
- Claims may be rejected or denied
- Reimbursement may be reduced
- Compliance risks may arise
Traditional billing often assumes coding has been performed correctly, even when errors exist.
Credentialing and Payer Alignment
If providers are not properly credentialed:
- Claims may be denied or processed as out-of-network
- Reimbursement may be reduced
- Services may not be billable
Billing teams typically identify these issues only after claims are submitted.
The Financial Impact of a Reactive Billing Model
When billing operates without control over upstream processes, organizations experience a reactive cycle:
- Claims are submitted
- Errors or misalignments are identified by the payer
- Claims are rejected or denied
- Billing teams correct and resubmit
- Payment is delayed
This cycle creates several challenges:
Increased Denial Rates
- Errors originating upstream lead to higher denial rates, increasing the workload on billing teams.
Delayed Cash Flow
- Each correction cycle delays reimbursement, impacting cash flow and financial stability.
Increased Administrative Costs
- Billing teams spend more time correcting errors rather than processing clean claims efficiently.
Revenue Leakage
- Some claims are never corrected or appealed, resulting in permanent revenue loss.
Why Billing Alone Cannot Maximize Revenue
Traditional medical billing is designed to process and collect revenue, not to ensure that revenue is generated correctly from the start.
This distinction is critical.
Billing teams can:
- Submit claims
- Follow up on payments
- Appeal denials
But they cannot fully control:
- Whether claims should have been submitted in the first place
- Whether services were authorized
- Whether documentation supports reimbursement
- Whether contracts allow payment
As a result, organizations that focus exclusively on billing improvements may see incremental gains but continue to experience recurring revenue challenges.
The Disconnect Between Billing and Revenue Performance
A common misconception is that improving billing performance will automatically improve overall revenue. In practice, billing performance and revenue performance are not always aligned.
For example:
- A billing team may achieve high claim submission accuracy
- Claims may be processed efficiently
- Payment posting may be timely
Yet revenue remains below expectations due to:
- Low reimbursement rates
- High denial rates
- Missing authorizations
- Incorrect patient eligibility
In these cases, billing is functioning correctly, but revenue performance is still limited by upstream factors.
The Role of Billing Within the Broader Revenue Cycle
Medical billing is a critical component of the healthcare revenue cycle, but it represents only one phase of a larger process.
The revenue cycle includes:
- Patient access and scheduling
- Eligibility verification
- Prior authorization
- Clinical documentation
- Coding and charge capture
- Claims submission and collections
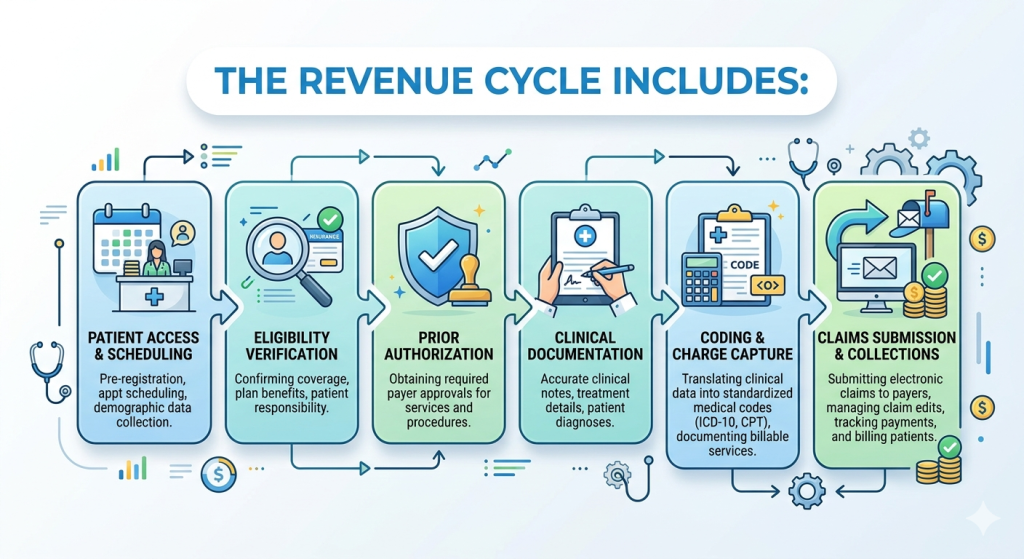
Billing operates within this cycle, but it does not control all of its components. For the revenue cycle to function effectively, each stage must be aligned.
When upstream processes are properly managed, billing teams can operate efficiently and focus on optimizing collections.
When upstream processes are misaligned, billing teams are forced into a reactive role, attempting to resolve issues that originated earlier.
Moving From Reactive to Preventive Revenue Management
Healthcare organizations that rely solely on traditional billing often operate in a reactive mode, addressing issues only after they appear in the claims process. A more effective approach involves shifting focus toward prevention.
This includes:
- Ensuring accurate eligibility verification before visits
- Obtaining required authorizations in advance
- Maintaining proper credentialing and payer alignment
- Strengthening documentation and coding practices
By addressing these factors earlier in the process, organizations can:
- Reduce denial rates
- Improve clean claim rates
- Accelerate reimbursement
- Reduce administrative workload
Billing teams can then focus on efficiency rather than correction.
Final Thoughts
Traditional medical billing remains an essential function within healthcare operations. It plays a critical role in converting services into revenue and ensuring that payments are collected.
However, billing alone cannot fully control revenue outcomes.
By the time a claim reaches the billing stage, many of the factors that determine reimbursement have already been set in motion.
Healthcare organizations that recognize the limitations of traditional billing and begin addressing the upstream drivers of revenue are better positioned to:
- Reduce denials
- Improve cash flow
- Increase reimbursement accuracy
- Strengthen overall financial performance
Evaluating Your Revenue Performance Approach
If your organization is experiencing persistent denials, delayed payments, or revenue that does not reflect the services you provide, it may be time to look beyond traditional billing processes.
L&C Advanced Practice Management works with healthcare organizations to identify where revenue challenges originate, strengthen upstream processes, and improve the systems that support financial performance.
To learn more, schedule a consultation with our team.
Frequently Asked Questions: traditional medical billing limitations
Traditional medical billing focuses only on post-service processes like claims submission and collections. It does not address upstream issues such as eligibility verification, prior authorization, or documentation errors, which significantly impact reimbursement.
Claims are often denied due to incorrect patient eligibility, missing prior authorization, coding errors, or insufficient clinical documentation, all of which occur before billing begins.
Medical billing is just one part of revenue cycle management. Revenue cycle management includes the entire process from patient scheduling and insurance verification to final payment collection.
Organizations can reduce denials by improving front-end processes such as eligibility verification, authorization workflows, accurate coding, and proper documentation.
Billing teams operate after key financial decisions are made. Without fixing upstream issues, billing can only react to problems, not prevent them.
L&C Advanced Practice Management helps healthcare organizations identify revenue gaps across the entire system, not just billing. By optimizing upstream processes like eligibility, authorization, documentation, and payer alignment, they help reduce denials, improve cash flow, and maximize reimbursement.