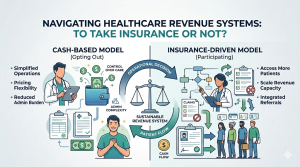
Revenue in healthcare is often misunderstood, and this misunderstanding is what leads to healthcare revenue leakage. It occurs when a healthcare practice earns revenue but fails to fully convert it into realized collections due to system breakdowns, denials, underpayments, coding errors, credentialing delays, and workflow inefficiencies across the revenue cycle. In simple terms, revenue in healthcare is the gap between what a practice should have been paid (potential revenue) and what it actually collects (realized revenue). Most practices fail to detect this leakage because they focus only on collections rather than evaluating the full revenue system, making it a hidden yet significant financial drain. Understanding how revenue in healthcare truly works, and measuring the gap between potential and realized revenue, is essential to identifying, diagnosing, and fixing revenue leakage.
Understanding Potential Revenue vs. Realized Revenue and Why Most Healthcare Practices Misunderstand Both
Many healthcare practices believe they have a revenue problem.
Revenue is down.
Payments are delayed.
Collections seem inconsistent.
Accounts receivable are growing.
When this happens, most organizations immediately start looking for quick explanations.
They assume the problem must be:
- The billing company
- The insurance companies
- The front desk
- Declining patient volume
- Reimbursement cuts
Sometimes those explanations are correct.
But more often, they are only surface, level interpretations of a deeper operational reality.
The truth is that many healthcare practices struggle financially, not because they lack effort or good intentions, but because they do not fully understand how revenue actually works in healthcare.
Revenue in healthcare is fundamentally different from revenue in most other industries. It behaves differently, it moves through a more complex system, and it is far more vulnerable to operational breakdowns.
Before a practice can diagnose revenue problems or fix them, it must first understand a foundational question:
What is revenue in healthcare?
And just as importantly: What is it not?
What Revenue in Healthcare Actually Is
At its core, healthcare revenue is the economic output created when clinical services are converted into financial reimbursement.
In simple terms, Healthcare revenue is the process of converting patient care into financial payment.
But this conversion is not automatic. Unlike most industries, healthcare revenue requires a complex operational system involving multiple steps, actors, and external organizations.
The journey from clinical service to payment typically includes:
- Patient scheduling and eligibility verification
- Documentation of the clinical encounter
- Coding and claim creation
- Claim submission to payers
- Adjudication by insurance companies
- Payment posting and reconciliation
- Denial management and recovery
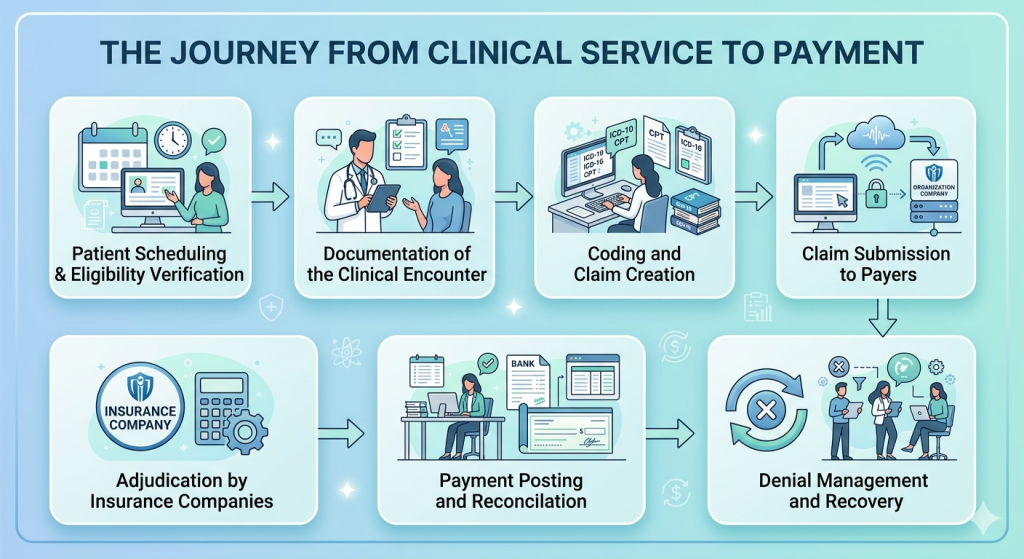
Each of these steps must work correctly for revenue to be fully realized.
If any part of the system fails, revenue does not simply slow down; it fractures.
What Revenue in Healthcare Is NOT
To understand healthcare revenue, it is equally important to understand what revenue is not.
Healthcare revenue is not: Revenue is NOT simply charges
Charges represent what a practice bills for services. But healthcare rarely pays based on charges. Payments are determined by:
- Payer contracts
- Fee schedules
- Allowed amounts
- Patient responsibility rules
A practice may charge $300 for a service and receive only $92. The charge is not revenue.
Revenue is NOT the same as collections
Collections represent money that has already arrived. But collections only tell us what happened after the system completed its process.
Collections do not reveal:
- How much revenue should have been earned
- Whether revenue was lost
- Whether revenue was delayed
- Whether revenue was under-collected
Collections are a result, not the full picture.
Revenue is NOT the same as profit
Revenue represents income generation, while profit represents what remains after expenses.
A practice can have high revenue but poor profitability if operational costs are excessive. Conversely, a practice can have low revenue but still maintain profitability through tight cost control.
Revenue and profit are related but fundamentally different metrics.
The Unique Nature of Healthcare Revenue
Healthcare revenue behaves very differently from revenue in most other industries. In many industries, revenue is realized immediately when a transaction occurs.
Examples include:
- Retail purchases
- Restaurant sales
- Software subscriptions
- Consulting services
A customer pays, and the revenue is immediately recognized.
Healthcare does not work this way. Healthcare revenue moves through a delayed, multi-party payment system.
Between the clinical service and final payment, there may be:
- Insurance verification processes
- Payer adjudication
- Claim edits and denials
- Patient billing cycles
- Appeals and reconsiderations
Because of this complexity, healthcare revenue exists in two fundamentally different forms.
The Two Types of Healthcare Revenue
To truly understand revenue in healthcare, leaders must recognize the difference between:
- Potential Revenue
- Realized Revenue
This distinction is the foundation for diagnosing revenue performance.
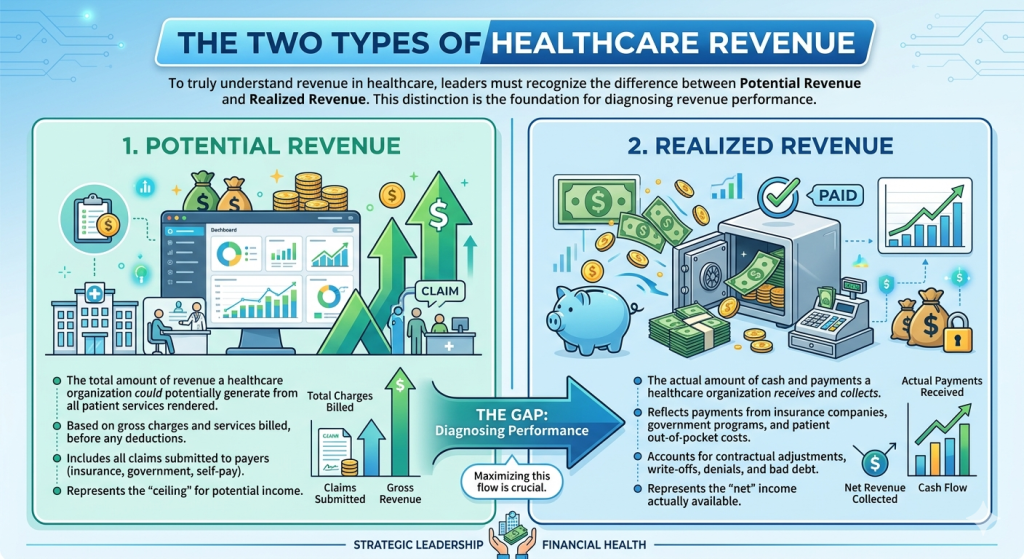
Potential Revenue
Potential revenue represents the total amount of revenue a practice has earned based on services provided and contractual reimbursement rates. It reflects what the practice should be paid if the revenue system functions correctly.
Potential revenue is determined by:
- The number of patient encounters
- The services performed
- The payer contracts in place
- The allowed reimbursement amounts
If a provider performs 100 services that should be reimbursed $120 each, the potential revenue equals:
$12,000
Potential revenue represents earned value. It is the financial output of clinical production.
Realized Revenue
Realized revenue represents the actual amount of money collected after the revenue system completes its process.
This includes payments from:
- Insurance companies
- Government payers
- Patient responsibility
- Secondary insurance
Realized revenue is the cash outcome of the revenue system.
Returning to the previous example:
Potential revenue: $12,000
But if the practice collects only $9,300 due to denials, underpayments, or operational failures, then:
Realized revenue = $9,300
The Revenue Performance Gap
The difference between potential revenue and realized revenue represents a critical performance indicator.
It shows how effectively the revenue system converts clinical services into financial outcomes.
Potential Revenue – Realized Revenue = Revenue Performance Gap
This gap may result from many causes, including:
- Credentialing issues
- Claim errors
- Payer underpayments
- Denial management failures
- Operational workflow breakdowns
Most practices focus only on collections and never examine the gap between what they should earn and what they actually collect.
This is one of the most common financial blind spots in healthcare.
Why This Concept Is Different From Other Industries
In most non-healthcare industries, potential revenue and realized revenue are nearly identical.
If a retail store sells a product for $50, the payment is received immediately. Potential revenue equals realized revenue. Healthcare breaks this rule.
Healthcare separates: production of services from the realization of payment. This separation introduces systemic complexity. It also introduces the possibility of system failure.
A healthcare practice can deliver services perfectly and still lose significant revenue if the operational systems responsible for converting those services into payment are flawed.
Why Most Healthcare Practices Misdiagnose Revenue Problems
One of the biggest challenges in healthcare revenue management is that most organizations attempt to diagnose revenue issues without understanding the structure of the revenue system itself.
As a result, practices often focus on symptoms rather than causes.
For example, a practice might notice that monthly collections have dropped and assume the problem must be:
- Poor billing performance
- Payer behavior
- Staff errors
- Declining patient demand
In response, leadership may attempt quick fixes such as:
- Replacing the billing company
- Hiring additional staff
- Blaming insurance companies
- Tightening operational policies
Sometimes these actions help. But often they do not.
The reason is simple. Many revenue problems are not isolated operational failures; they are signals that the revenue system itself is misaligned or structurally weakened.
Without understanding the difference between potential revenue and realized revenue, organizations cannot accurately determine:
- How much revenue should exist
- Where revenue is being lost
- Why do those losses occur
When leaders only look at collections, they are essentially trying to diagnose a complex system while seeing only the final output.
This is why revenue problems often persist even after multiple operational changes. The underlying causes remain hidden.
The Hidden Danger: Revenue Problems
When the revenue system fails to convert potential revenue into realized revenue, revenue problems begin to appear.
These problems often manifest as symptoms such as:
- Declining revenue
- Inconsistent monthly income
- Delayed payments
- Increasing accounts receivable
- Growing denial rates
Many practices treat these symptoms as isolated issues. But these symptoms are usually signals of deeper structural problems within the revenue system.
These signals are what we call revenue problems. Revenue problems represent the visible manifestations of revenue system failure.
They are what leadership notices first.
The Deeper Issue: Revenue Fractures
Behind every persistent revenue problem lies something deeper.
Operational systems do not simply produce problems by accident. They produce problems because something in the system has structurally broken down. These structural breakdowns are what we refer to as revenue fractures.
Revenue fractures are:
- Underlying structural weaknesses
- Systemic misalignments
- Operational design failures
They exist beneath the surface of day-to-day financial results. While revenue problems are the symptoms, revenue fractures are the structural causes. Understanding this distinction is critical for healthcare leaders.
If a practice only addresses the visible revenue problems without identifying the underlying fractures, the problems will eventually return.
Final Thought
Revenue in healthcare is not just a financial metric. It is the output of an operational system.
When that system is designed correctly and executed effectively, potential revenue converts into realized revenue with minimal loss.
But when the system fractures, revenue problems inevitably follow.
Understanding the difference between potential revenue, realized revenue, revenue problems, and revenue fractures is essential for healthcare leaders who want to truly understand the financial performance of their organizations.
Without this clarity, practices often focus only on surface-level financial outcomes, such as monthly collections, without recognizing the deeper operational systems that ultimately determine revenue success or failure.
When healthcare organizations begin to think about revenue not just as money collected, but as the result of a complex operational system, they gain the ability to diagnose problems more accurately, identify hidden revenue losses, and build systems that support stable, predictable financial performance.
For healthcare practices that want to grow, scale, or simply stabilize their financial outcomes, this shift in perspective is not optional.
It is foundational. If your organization suspects that revenue is being lost somewhere in the process of converting clinical services into payment, a structured revenue diagnostic can help uncover where the breakdowns are occurring.
Learn more or schedule a conversation with the revenue specialists at L&C Advanced Practice Management.
Healthcare revenue cycle management (RCM) is the process of managing financial transactions from patient scheduling to final payment collection.
Potential revenue = Maximum possible earnings based on services provided Realized revenue = Actual collected payments
Common reasons include:
- Poor eligibility verification
- Coding errors
- Documentation gaps
- Claim denials
No. Billing companies can only optimize collections. Most revenue issues originate before billing begins.
Optimize front-desk processes Improve documentation accuracy Implement coding audits Monitor KPIs across the revenue cycle
L&C Advanced Practice Management helps healthcare organizations identify hidden revenue leaks by analyzing the entire patient journey—from scheduling to collections. Instead of focusing only on billing, L&C builds a complete revenue optimization system, improving both operational efficiency and financial performance.