
Healthcare organizations today face an increasingly complex financial environment. Rising claim denials, payer scrutiny, regulatory complexity, and staffing shortages have placed enormous pressure on revenue cycle teams. At the same time, healthcare providers are expected to operate with the same level of operational efficiency and financial discipline seen in other industries.
These pressures have accelerated the adoption of Revenue Cycle Management – RCM automation software.
Automation technologies powered by artificial intelligence (AI), robotic process automation (RPA), analytics, and cloud-based integrations are transforming how healthcare organizations manage billing, claims, and reimbursement. These systems promise faster collections, improved financial transparency, and reduced administrative workload.
However, automation is not a perfect solution. While RCM automation software can significantly improve efficiency, it also has limitations that healthcare organizations must understand before relying too heavily on automated processes.
This article explores what RCM automation software is, how it works, the financial and operational benefits it offers, the costs of implementation, and the areas where automation still struggles to replace the expertise of experienced revenue cycle professionals.
What is RCM Automation Software?
Revenue Cycle Management (RCM) refers to the financial processes that healthcare organizations use to track patient care from the initial appointment through final payment collection.
The revenue cycle typically includes several operational stages:
- Patient scheduling
- Insurance eligibility verification
- Prior authorization
- Medical coding
- Claims submission
- Payment posting
- Rejection management
- Denial management
- Patient billing and collections
RCM automation software uses technology to streamline many of these administrative processes. By automating repetitive tasks, healthcare organizations can reduce manual workload while improving consistency and speed across revenue cycle operations.
Modern automation platforms often integrate with:
- Electronic Health Records (EHRs)
- Practice Management Systems
- Clearinghouses
- Insurance payer portals
- Payment processing systems
These integrations allow financial and clinical workflows to operate in a connected environment where large volumes of data can be processed efficiently.
Common automation capabilities include:
- Automated eligibility verification
- Claims scrubbing and electronic submission
- ERA-based payment posting
- Claim status tracking
- Rejection categorization
- Denial analytics
- Patient billing automation
In many organizations, RCM automation systems function as the operational infrastructure supporting the entire revenue cycle.
The RCM Automation Workflow: Where Automation Fits in the Revenue Cycle
To understand the role of automation in revenue cycle management, it helps to view the revenue cycle as a connected operational workflow. Each stage presents opportunities for automation to improve efficiency, reduce errors, and accelerate reimbursement.
Most healthcare organizations operate a revenue cycle that includes the following stages.
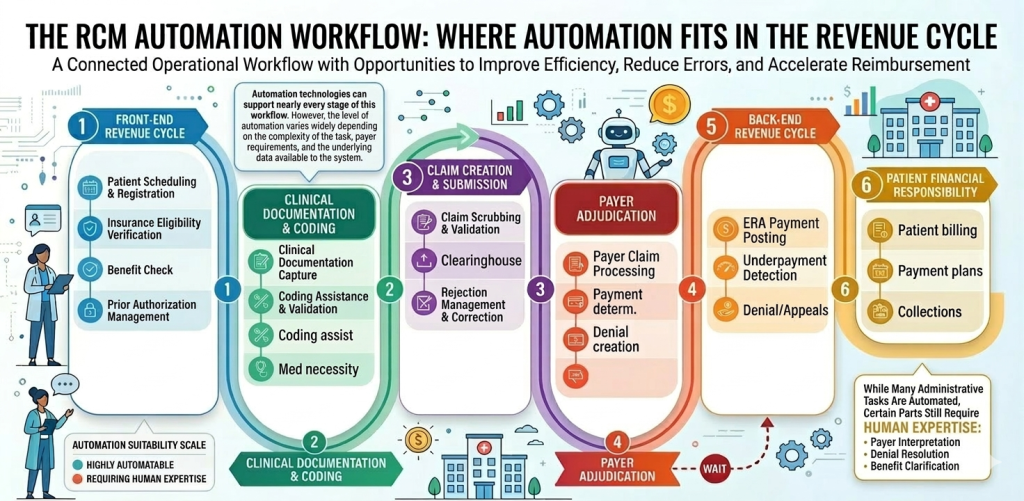
Front-End Revenue Cycle
- Patient scheduling and registration
- Insurance eligibility verification
- Benefit checks
- Prior authorization management
Clinical Documentation and Coding
- Clinical documentation capture
- Coding assistance and validation
- Medical necessity verification
Claim Creation and Submission
- Claim scrubbing and validation
- Clearinghouse submission
- Rejection management and correction
Payer Adjudication
- Payer claim processing
- Payment determination
- Denial generation
Back-End Revenue Cycle
- ERA payment posting
- Underpayment detection
- Denial management and appeals
Patient Financial Responsibility
- Patient billing
- Payment plans
- Collections and follow-up
Automation technologies can support nearly every stage of this workflow. However, the level of automation varies widely depending on the complexity of the task, payer requirements, and the underlying data available to the system.
While many administrative tasks can be automated effectively, certain parts of the revenue cycle—particularly those involving payer interpretation, denial resolution, and benefit clarification—still require human expertise.
Why RCM Automation Is Growing Rapidly
Healthcare reimbursement has become increasingly complex over the past decade. Providers must navigate expanding payer policies, authorization requirements, documentation standards, and billing regulations.
Several industry trends have increased the importance of efficient revenue cycle management:
- Rising claim denial rates
- Increasing patient financial responsibility
- Growing payer administrative requirements
- Shortages of experienced billing staff
- Increased regulatory oversight
- Expansion of value-based reimbursement models
Healthcare organizations process thousands—or even millions—of financial transactions every year. Many of these processes involve repetitive administrative steps that can be performed more efficiently through automation.
RCM automation software allows healthcare organizations to process these tasks faster and with greater consistency than traditional manual workflows.
For organizations operating with tight margins, even small improvements in revenue cycle efficiency can produce meaningful financial gains.
Key Areas Where RCM Automation Is Used
RCM automation platforms support multiple stages of the revenue cycle. While capabilities vary across systems, automation tools are commonly used in several operational areas.
One of the most common uses of RCM automation is insurance eligibility and benefit verification.
Automation systems can retrieve insurance data from payer systems or clearinghouses to confirm:
- Active insurance coverage
- Deductible balances
- Co-pay amounts
- Coinsurance levels
- Coverage start and end dates
This automation reduces the need for manual payer portal checks or phone calls to insurance companies and allows front-office teams to verify coverage quickly.
Some RCM automation systems include AI-assisted coding tools that analyze clinical documentation and suggest billing codes.
These tools can help identify:
- Potential CPT and diagnosis codes
- Missing documentation elements
- Medical necessity alerts
- Compliance risks
Automation can improve coding efficiency and reduce errors, although final coding decisions still require experienced coding professionals.
Claims submission is one of the most widely automated areas of the revenue cycle.
Automation systems can:
- Scrub claims for formatting errors
- Identify missing required data elements
- Automatically submit claims to clearinghouses
- Track claim status updates
These capabilities help improve the clean claim rate, meaning a higher percentage of claims are accepted on the first submission.
Higher clean claim rates reduce resubmission workload and accelerate reimbursement timelines.
Claim rejections occur before a claim enters the payer’s adjudication system. Most rejections originate from clearinghouse edits or payer front-end claim validation systems.
Common rejection causes include:
- Missing patient demographics
- Invalid provider identifiers
- Incorrect payer routing
- Formatting errors in claim fields
- Missing authorization numbers
Automation tools help identify these issues before claims are submitted through claim scrubbing technology.
Automated claim edits review claim data against payer rules and clearinghouse requirements, allowing billing teams to correct errors before submission.
When implemented effectively, automation significantly reduces rejection rates and improves operational efficiency.
Denials occur after a payer has received and adjudicated a claim but has determined that payment will not be issued.
Common denial reasons include:
- Lack of medical necessity
- Missing or invalid authorization
- Non-covered services
- Benefit limitations
- Credentialing or network participation issues
- Timely filing violations
Automation tools assist denial management by:
- Categorizing denial codes
- Identifying denial patterns
- Tracking appeal timelines
- Prioritizing high-value claims for follow-up
While automation can organize denial information, resolution often requires manual investigation and payer communication.
Payment posting is another area where automation significantly improves efficiency.
Electronic Remittance Advice (ERA) files allow systems to automatically record payments and adjustments directly into billing platforms.
Automated ERA posting can:
- Match payments to claims
- Apply contractual adjustments
- Assign patient responsibility balances
This reduces manual data entry and improves financial reporting accuracy.
Automation also supports patient billing workflows through tools such as:
- Online patient billing portals
- Automated billing notifications
- Digital payment processing
- Payment plan management
These tools improve payment convenience for patients while reducing administrative workload for billing teams.
When implemented effectively, RCM automation can improve several financial performance indicators.
These benefits include:
Improved clean claim rates: Automated claim scrubbing reduces submission errors.
Faster reimbursement timelines: Automation accelerates claim submission and payment posting.
Improved revenue capture: Automation tools can identify underpayments and missing charges.
Reduced administrative costs: Organizations can process higher volumes of transactions without increasing staffing levels proportionally. Even small improvements in denial rates or reimbursement speed can produce substantial financial gains.
Automation improves operational efficiency by reducing repetitive administrative work.
Revenue cycle teams can focus on higher-value activities such as:
- Denial resolution
- payer communication
- financial analysis
- compliance monitoring
Automation also provides leadership with improved visibility into revenue cycle performance through analytics dashboards that track metrics such as denial rates and days in accounts receivable.
Where RCM Automation Still Falls Short
Despite its advantages, RCM automation software has important limitations.
Automation systems process structured data efficiently but often struggle to interpret the complexity of payer systems and healthcare reimbursement rules.
Automated eligibility checks may confirm active coverage, but often assume the provider is in-network unless further verification occurs. They may also fail to identify specialty-specific plan limitations, such as visit caps or authorization requirements.
Automation also frequently cannot determine the true claims administrator when policies involve delegated medical groups, carve-outs, or third-party administrators.
ERA payment posting automation can misallocate payments when claims contain multiple service lines or complex adjustment patterns.
Additionally, denial codes returned in ERAs are often not descriptive enough to resolve issues without additional investigation, requiring staff to review payer portals or contact insurers directly.
These limitations highlight an important reality: automation can process large amounts of data quickly, but it cannot always interpret payer behavior accurately.
For this reason, automation should be viewed as a support tool rather than a replacement for experienced revenue cycle oversight.
The Cost of Implementing RCM Automation
RCM automation software costs vary depending on organization size and system complexity.
Common pricing models include:
- Monthly subscription fees
- Per-provider licensing
- Transaction-based pricing
- Percentage-of-collections pricing
Small practices may spend several hundred to several thousand dollars per provider per month, while enterprise health systems may invest hundreds of thousands annually.
Implementation also requires operational investment, including:
- System integration
- Workflow redesign
- Staff training
- Configuration and testing
Automation initiatives typically require several months of planning before full deployment.
Can RCM Automation Replace RCM Staff?
RCM automation works best in high-volume, rules-based tasks such as eligibility queries, claim formatting checks, automated submission, and basic payment posting.
However, many revenue cycle activities require investigation, interpretation, and payer communication.
These include:
- Complex denial appeals
- Payer contract interpretation
- Benefit clarification
- Claims research
- Compliance monitoring
Automation can reduce administrative workload, but cannot replace the expertise required to navigate healthcare reimbursement complexities.
In most organizations, automation shifts staff toward more analytical and problem-solving roles rather than eliminating positions entirely.
Final Thoughts
RCM automation software is transforming healthcare finance by improving efficiency and enabling organizations to process financial transactions at a greater scale.
When implemented effectively, automation can reduce administrative workload, accelerate reimbursement timelines, and improve financial transparency.
However, automation also has clear limitations. Eligibility verification may assume in-network status, overlook specialty-specific plan restrictions, or fail to identify the correct claims administrator. ERA payment posting may misallocate payments across service lines, and denial codes often require manual investigation.
For these reasons, automation should be viewed as a powerful operational tool—but not a replacement for experienced revenue cycle professionals.
Healthcare organizations that combine advanced automation technology with knowledgeable revenue cycle teams will be best positioned to navigate the growing complexity of modern healthcare reimbursement.
Want to Evaluate Whether RCM Automation Is Actually Working for Your Practice?
Many of the revenue cycle problems healthcare organizations experience today are not caused by staff performance but by hidden workflow gaps between automation systems, payer rules, and operational processes.
If your organization is evaluating RCM automation tools—or if you already use automation but still experience issues with denials, payment posting accuracy, or reimbursement delays—it may be helpful to take a closer look at how your revenue cycle is functioning as a system.
At L&C Advanced Practice Management, our revenue cycle specialists work with healthcare organizations to analyze billing workflows, payer behavior, and automation performance across the entire revenue cycle.
During a Revenue Cycle Diagnostic Call, our team can help review:
- Claim rejection and denial trends
- Automation workflow gaps
- Eligibility and benefit verification processes
- ERA posting and reconciliation accuracy
- Opportunities to improve reimbursement performance
Schedule a Revenue Cycle Diagnostic Call with an L&C revenue cycle specialist to explore how your current systems and workflows may be impacting your financial performance.
Because sometimes the issue isn’t the technology itself — it’s how the system is configured, integrated, and managed.
Frequently Asked Questions About RCM Automation
RCM automation software is a technology platform that automates administrative and financial tasks within the healthcare revenue cycle. It helps healthcare organizations streamline processes such as insurance eligibility verification, medical coding assistance, claims submission, payment posting, denial tracking, and patient billing. By reducing manual work and improving workflow efficiency, RCM automation software helps providers accelerate reimbursements and reduce billing errors.
The main benefits of RCM automation software include faster claim processing, improved clean claim rates, reduced administrative workload, and better financial visibility. Automation tools can quickly verify insurance eligibility, scrub claims for errors, submit claims electronically, and automatically post payments from ERA files. These capabilities help healthcare organizations reduce denials, improve cash flow, and operate more efficiently.
L&C Advanced Practice Management helps healthcare organizations evaluate and optimize their revenue cycle workflows, including how RCM automation software is configured and used. Their revenue cycle specialists analyze claim rejection trends, denial patterns, eligibility verification processes, and ERA payment posting accuracy to identify gaps that automation alone may not detect. Through a Revenue Cycle Diagnostic Call, healthcare providers can gain insights into workflow inefficiencies and opportunities to improve reimbursement performance while ensuring automation tools are supporting—not disrupting—the revenue cycle.




